Mount Sinai Researchers Identify Mechanisms and Potential Biomarkers of Tumor Cell Dormancy
May be able to recreate conditions that keep cancer cells from growing after they have spread.
Oncologists have long puzzled over the fact that after cancer treatment, single cancer cells that are dispersed throughout the body – so-called disseminated tumor cells – are quick to grow and form secondary tumors called metastases in certain organs, while in other organs they metastasize more slowly, sometimes decades later. Such is the case with head and neck squamous cell carcinoma (HNSCC) cells, which remain dormant when lodged in bone marrow but rapidly form tumors when they make their way into the lungs.
A study published online October 27 by Nature Cell Biology by Bragado et al. reveals that bone marrow contains high levels of TGFβ2, which activates the tumor suppressor gene p38 in tumor cells and triggers a cascade of events that renders tumor cells dormant and keeps HNSCC growth in check. In the lungs, where TGFβ2 is in short supply, these cells rapidly form tumors.
The research team, led by Julio A. Aguirre-Ghiso, PhD, Associate Professor of Medicine, Hematology and Medical Oncology, and Otolaryngology at the Icahn School of Medicine at Mount Sinai, is the first to identify the role of TGFβ2 in determining whether HNSCC cells will remain harmlessly dormant or behave aggressively in a given location. The study confirms a century-old theory called the "seed and soil" theory of metastasis, which suggests that a tumor cell – the seed – either sleeps or thrives within the unique environment of each organ – the soil.
"Our study provides critical evidence to explain why tumor cells gain a firm foothold in certain organs but not in others, where they can remain inactive for long periods of time," explained Dr. Aguirre-Ghiso.
Approximately 80 percent of the animal models the researchers studied contained disseminated HNSCC cells in the lungs, while less than 30 percent contained tumor cells in the bone marrow. After removing the primary tumors, the number of disseminated tumor cells in the bone marrow remained the same for several weeks (equivalent to ~ 3 years in humans). However, the number of tumor cells in the lungs increased shortly after the tumors were removed, suggesting that conditions within each organ had a long-lasting effect on the cells’ behavior.
In addition, the researchers discovered that lowering TGFβ2 or p38 levels awakened dormant cells and fueled metastatic growth throughout the body.
These findings may have implications for estrogen-positive breast tumor cells, which have a similar genetic signature to that of dormant HNSCC cells.
"Our study is the first to identify specific characteristics found in cancer cells as well as in the microenvironment in which they are found that determine whether they will metastasize rapidly, posing a new threat to the patient, or will remain dormant for a period of time," said Dr. Aguirre-Ghiso. "Eventually, we may be able to predict, based on markers detected in disseminated tumor cells and/or in the microenvironment, which patients have a dormant disease and which ones will need more aggressive treatment. This information may also lead to the development of new drugs that mimic the pathways that prevent tumor cells from metastasizing."
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with 48,000 employees working across seven hospitals, more than 400 outpatient practices, more than 600 research and clinical labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time—discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 9,000 primary and specialty care physicians and 10 free-standing joint-venture centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida. Hospitals within the System are consistently ranked by Newsweek’s® “The World’s Best Smart Hospitals, Best in State Hospitals, World Best Hospitals and Best Specialty Hospitals” and by U.S. News & World Report's® “Best Hospitals” and “Best Children’s Hospitals.” The Mount Sinai Hospital is on the U.S. News & World Report® “Best Hospitals” Honor Roll for 2025-2026.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Instagram, LinkedIn, X, and YouTube.
Mount Sinai Study May Help Cancer Patients Keep Their Bladder
Feb 19, 2026 View All Press Releases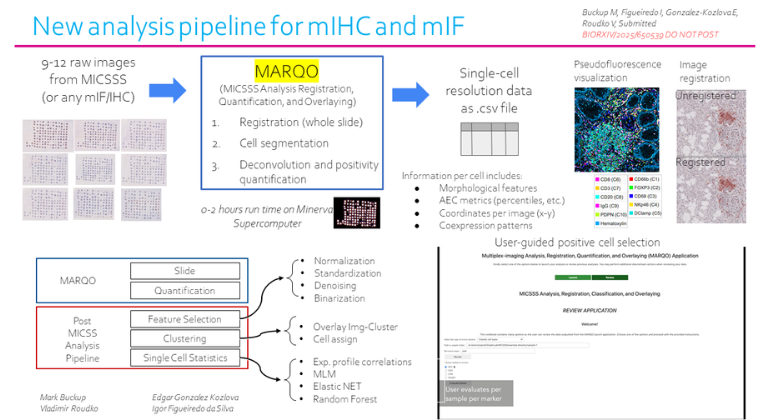
Mount Sinai Scientists Create AI-Powered Tool to Improve Cancer Tissue Analysis
Aug 25, 2025 View All Press Releases